Floaters Unveiled: Solutions for a Clearer View
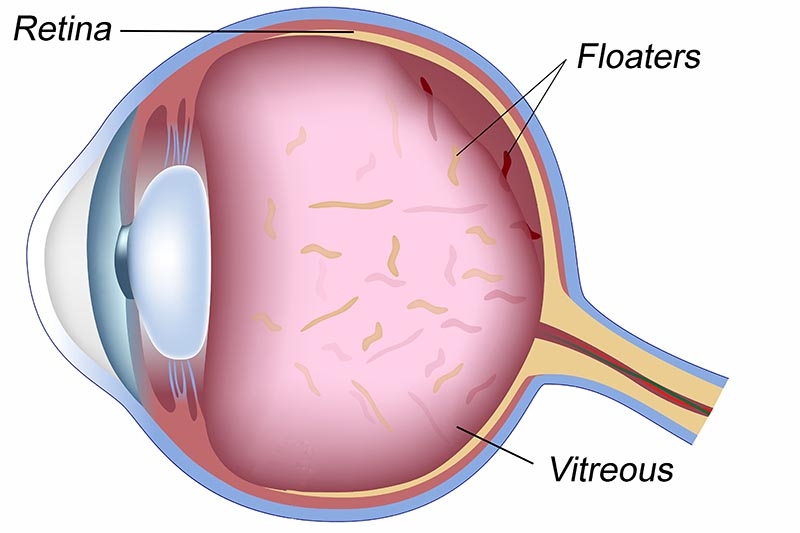
Eye floaters are tiny, cloudy, clumps of cells that appear in the otherwise clear fluid (vitreous) that fills the back three-fourths of the eye. They are sometimes called Vitreous Floaters or vitreous opacities.
Eye floaters that are not close to other ocular structures are ideal for laser treatment because they have no blood supply and can not bleed. The floaters are vaporized, not broken into smaller floaters.
Eye Exams
Eye Care
Lenses

DR. corrales
People see eye floaters as small specks, cobwebs, or clouds moving in their field of vision. They range from being a nuisance that can be ignored, to interfering with essential daily activities such as reading or driving.

Types of eye floaters and success rates
Discover the Main Types of Eye Floaters We Encounter. By delving into this information, you’ll gain insight into the types of floaters you might be experiencing and their success rates in treatment. However, classifying your own floater can be challenging. While an ophthalmologist’s assessment provides more clarity, since this procedure is relatively unfamiliar, the most reliable evaluation comes from a surgeon skilled in this treatment.
Our laser treatment boasts an impressive overall success rate of approximately 92%. However, success rates vary depending on the type of floater. For the 8% of patients who experienced no improvement, no evidence of the procedure was found, ensuring no harm was done.
Weiss Ring:
Common in patients 55 years or older, caused by a posterior detachment of the vitreous jelly. Often appears as a vague glob and can be completely vaporized with laser in about 98% of cases.
Dots and Lines Near the Retina
Sometimes seen in patients younger than 55 years as distinct dots and lines very near the retina, making them very bothersome to patients. They may be difficult to treat with laser if too close to the retina.
Vitreous Degeneration
Common in patients 55 years or younger, caused by early marked degeneration of the vitreous, resulting in floaters resembling cobwebs or clouds.
Floater Duet
A combination of a floater caused by a posterior vitreous detachment and multiple floaters low in the vitreous due to vitreous degeneration. Treatable with laser if the main offender is the floater pulled off the back of the eye.

Eye floaters and
the US Food and Drug administration
For years, YAG lasers have been used to treat vitreous floaters. However, the FDA had not previously addressed floater treatment, lacking submitted data.
In 2002, Dr. Karickhoff submitted a comprehensive document to the FDA, outlining laser effects, studies, and expertise. The FDA ruled his proposed study as non-significant risk, waiving the need for special device exemption.
Dr. Karickhoff’s formal study, initiated after FDA approval, concluded three years later. Despite positive rulings, it’s important to note that laser treatment of eye floaters remains an off-label use of the YAG laser.
Laser disruption is accomplished as follows. After dilating the pupil, a numbing eye drop is given and a special contact lens for treating eye floaters is placed on the eye. Then the laser is carefully aimed, and the floater or floaters are either vaporized with the laser, or the floater’s attachments are vaporized so that the floater is re-positioned to a different part of the eye. This disruption also helps the eye to absorb any remaining particles. After vaporizing the big floater or floaters, we may have to leave tiny particles that are just too small to aim on.
Laser Procedure Actually Gets Rid of Eye Floaters
The laser procedure effectively removes eye floaters instead of just breaking them into smaller pieces, using a technique called optical breakdown. Unlike vitrectomy, this method is more precise and safer as it does not require opening the eye, significantly reducing the risk of complications such as infections, wound leaks, and retinal detachment.
The science background for laser treatment of eye floaters
Contrary to common perception, the laser doesn’t break floaters into smaller particles but largely obliterates them so they cease to exist. However, at the procedure’s end, especially with multiple floaters, some particles may remain too close to the retina to treat or are simply too small to target.
Optical breakdown requires:
- a very high frequency (changing from plus to minus) electrical field in the optical region of the electromagnetic spectrum that
- is confined to a very small area.
When achieved, upon firing the laser, the clear vitreous and floater become opaque (plasma formation) at a microscopic point. They absorb laser energy, producing a micro lightning flash (optical breakdown). This flash obliterates the floater with a combination of photochemical, thermal, thermoacoustical, and electromagnetic optical field effects. Each time optical breakdown occurs, the surgeon sees the micro lightning on the surface of the floater, and both the surgeon and the patient hear the acoustical component (a micro thunder snap).
To focus this force on the floater and to control it:
- The surgeon has perfect microscopic viewing of the floater and the laser aiming beam,
- He has precise control of the laser power,
- The field size of the focused laser beam is only 8 microns wide in air and is much smaller than that when we use one of our three focusing contact lenses during surgery, and
- The laser pulse duration of our modern laser (produced in 1999) is only 4 nanoseconds (10 to the minus 9 seconds). Total duration of treatment per case is usually only about 160 nanoseconds.
Cost and Payment
The initial consultation evaluates your floaters, including a history, eye health examination, and necessary retinal tests.
Fees are submitted to your insurance company if applicable.
Initial Consultation
$300.00
Laser Treatment fee (per eye)
$2,000.00
The Laser treatment fee (not covered by insurance):
- Covers two treatments per eye during your visit.
- Additional treatments may be necessary for large or multiple floaters.
- Additional treatment within the first twelve months: $500 per session.
- After one year: $300 for an examination plus $1,000 for each additional laser treatment if done.
The payment policy
- Payment for laser treatment is requested at the time of service, even if you have insurance.
- Insurance companies may not fully cover the procedure due to its classification as experimental.
- Reimbursement varies, with some insurance companies not covering the procedure.
- Patients are responsible for the full laser fee payment and are required to sign a form acknowledging this.
Insurance participation
- We participate with select insurance companies for the examination and retinal tests. Insurances We Participate With
- Please check with our office for details on insurance participation.
Candidate for a laser treatment of eye floaters?
While some floaters may naturally absorb or move out of sight over time, others persist and can significantly disrupt daily activities such as reading, driving, or working on a computer. In such cases, treatment can be beneficial.
Ideal Candidates For Laser Treatment
The ideal candidates for laser treatment of floaters typically:
- Have developed their floater due to a vitreous detachment.
- Have a small number of floaters.
- Have floaters located away from the lens and the retina.
Factors that contraindicate laser treatment of eye floaters
Laser treatment for eye floaters may not be offered to certain individuals. This includes those with asteroid hyalosis or active eye inflammation, as well as patients with floaters and membranes from vitreous hemorrhage, which may require a surgical procedure with significant risks. Additionally, patients with elevated eye pressure or glaucoma may be ineligible for the procedure. Psychological factors, such as excessive anxiety or depression due to floaters, or a history of psychiatric problems, may also impact candidacy for laser treatment.
Young patients with eye floaters
Some floaters in patients under 35 cannot be treated. If you are under 35, please read sections (B) and (C) on our “Floater Types – Success” webpage for relevant information. We offer evaluation appointments for younger patients but require a signed note from an eye doctor confirming visibility of the floaters to schedule treatment. This note can be mailed or faxed. If planning a trip for both evaluation and treatment, ensure we receive the doctor’s note before scheduling treatment appointments.
Other treatment
We seldom recommend vitrectomy for isolated vitreous floaters due to high complication rates. About 50% of patients over 50 develop cataracts within five years, with lower rates under 50. Other risks include retinal tears, detachment, infection, and leaks from incisions. Despite these risks, vitrectomy is vital for treating certain eye diseases.
Vitrectomy can remove all vitreous and floaters but often removes more vitreous than necessary, aiming to eliminate floaters. The technique was refined at Duke University Eye Center, where Dr. Karickhoff trained and serves on the Advisory Board.
Our laser
After extensive study and testing, we purchased what we believe to be the finest laser available for this procedure.
YAG Laser Requirement for Floaters
For effective floater treatment, the YAG laser’s treatment beam must be nearly parallel to the illumination beam. Misalignment renders the laser ineffective for floaters in the middle and back of the eye. Many YAG lasers are designed for cataract treatment and are unsuitable for floaters. Specialists in floater treatments use the appropriate lasers.

Our Surgical Contact Lenses
We offer a comprehensive series of seven surgical contact lenses for floater laser treatment, widely used and sold internationally by a top manufacturer.
Benefits of Surgical Contact Lenses:
Optical Neutralization
Stabilizes Eye Movement
Corrects Aberrations
Enhanced Laser Focus
Custom Focus
Our Advanced Lenses
Our lenses, including the specialized Karickhoff Lenses, are designed to optimize the effectiveness and safety of floater laser treatments. Our collection includes off-axis lenses that facilitate treatment of floaters that are not exactly in the center.
World literature a Listing abstract notes
A search through our hospital library, Med-Line source, and the National Library of Medicine reveals only five papers in the literature on treatment of vitreous floaters. They are listed below. The total number of floater cases reported is 60.There were no serious complications in any of the floater disruption cases. Only the Aron-Rosa paper has long term follow-up. In that paper there were no late onset complications. Doctor Karickhoff’s book is the only one that has been written on the subject of laser treatment of vitreous floaters.
Vitreolysis with the Q-switched laser
Fankhauser, Franz “Vitreolysis with the Q-switched laser” Arch Ophthalmology 1985 103:1166-1171
Dr. Fankhauser is considered the founder of the laser treatment of floaters.His paper consists of mainly cutting vitreous membranes, but there are 10 cases of floater disruption. There were no complications.
Q-Switched neodymium: YAG laser surgery of the vitreous
Little, H. L. “Q-Switched neodymium: YAG laser surgery of the vitreous” Graefe’s Arch Clin Exp Ophthalmol 1986 224: 240-246
This study of 59 cases included 25 cases of vitreous opacities. Other cases were of vitroretinal band and membranes. No complications were listed for the treatment of vitreous opacities cases. They used a modified Coherent model 9900 laser. He stresses the importance of using contact lenses with magnification.
Indications for Q-switched and mode-locked Nd:YAG lasers in vitreoretinal pathology
Tassignon, MJ “Indications for Q-switched and mode-locked Nd:YAG lasers in vitreoretinal pathology“, European Journal of Ophthalmology 1991; vol. 1/no. 3: 123-130
This is a comparison of the two laser types mainly for cutting vitreous membranes. The treatment of 3 floaters, all severe, was reported.The Q-switched laser was used. All cases were successfully treated and there were no complications reported.
Treatment of vitreous floaters with neodymium YAG laser
Tsai, Wu-Fu “Treatment of vitreous floaters with neodymium YAG laser“, British Journal of Ophthalmology 1993; 77:485-488
This is the only report in the literature containing only treatment of vitreous floaters cases. It reports 15 cases of obliteration of vitreous floaters with the Lasag Microruptor III YAG laser. All cases were successful and there were no complications. Patients were chosen because the floaters caused psychological symptoms. 13 of their cases had a PVD.
World literature a Listing abstract notes
A search through our hospital library, Med-Line source, and the National Library of Medicine reveals only five papers in the literature on treatment of vitreous floaters. They are listed below. The total number of floater cases reported is 60.There were no serious complications in any of the floater disruption cases. Only the Aron-Rosa paper has long term follow-up. In that paper there were no late onset complications. Doctor Karickhoff’s book is the only one that has been written on the subject of laser treatment of vitreous floaters.
Vitreolysis with the Q-switched laser
Fankhauser, Franz “Vitreolysis with the Q-switched laser” Arch Ophthalmology 1985 103:1166-1171
Dr. Fankhauser is considered the founder of the laser treatment of floaters.His paper consists of mainly cutting vitreous membranes, but there are 10 cases of floater disruption. There were no complications.
Q-Switched neodymium: YAG laser surgery of the vitreous
Little, H. L. “Q-Switched neodymium: YAG laser surgery of the vitreous” Graefe’s Arch Clin Exp Ophthalmol 1986 224: 240-246
This study of 59 cases included 25 cases of vitreous opacities. Other cases were of vitroretinal band and membranes. No complications were listed for the treatment of vitreous opacities cases. They used a modified Coherent model 9900 laser. He stresses the importance of using contact lenses with magnification.
Indications for Q-switched and mode-locked Nd:YAG lasers in vitreoretinal pathology
Tassignon, MJ “Indications for Q-switched and mode-locked Nd:YAG lasers in vitreoretinal pathology“, European Journal of Ophthalmology 1991; vol. 1/no. 3: 123-130
This is a comparison of the two laser types mainly for cutting vitreous membranes. The treatment of 3 floaters, all severe, was reported.The Q-switched laser was used. All cases were successfully treated and there were no complications reported.
Treatment of vitreous floaters with neodymium YAG laser
Tsai, Wu-Fu “Treatment of vitreous floaters with neodymium YAG laser“, British Journal of Ophthalmology 1993; 77:485-488
This is the only report in the literature containing only treatment of vitreous floaters cases. It reports 15 cases of obliteration of vitreous floaters with the Lasag Microruptor III YAG laser. All cases were successful and there were no complications. Patients were chosen because the floaters caused psychological symptoms. 13 of their cases had a PVD.
Oftalmology website links
American Society of Cataract and Refractive Surgeons (ASCRS)
This is a good site to find an ophthalmologist in your area. I believe their members tend to be well informed on the latest advances in cataract and refractive surgery.
Duke University Eye Center
Many of the instruments and the technique for vitrectomy (removal of the vitreous) were developed at Duke University where Doctor Karickhoff trained and remains on the Advisory Board. A large Eye Research Institute was added in 2005. Dr. Karickhoff gave the medical lecture for the opening of this Institute.
National Library of Medicine
This site makes available the Medline search and other databases at the National Library of Medicine. You can do free on-line literature search.
Prevent Blindness America
An informative site where you can download several vision self-tests for adults and children.
Quackwatch
Ophthalmology is not immune from the enormous amount of quackery, fraud, and false claims in medicine. See at the “Eye-Related Quackery” page.
Research in Vision and Ophthalmology
This site is helpful in learning the latest research in vision and ophthalmology.
Free Book:
Laser Treatment for Eye Floaters
This is the world’s first and only physician-authored book on this subject. Based on over 6,000 procedures by John Karickhoff, M.D., it has taught over 500 eye surgeons worldwide. Now retired, Dr. Karickhoff offers the updated e-book for free, featuring 112 colored illustrations (up from 36) and an improved index highlighting 24 essential topics.
This is the world’s first and only physician-authored book on this subject. Based on over 6,000 procedures by John Karickhoff, M.D., it has taught over 500 eye surgeons worldwide. Now retired, Dr. Karickhoff offers the updated e-book for free, featuring 112 colored illustrations (up from 36) and an improved index highlighting 24 essential topics.